Melasma Treatment at Charlotte Skin & Laser
Fade Dark Spots: Advanced Solutions for Melasma
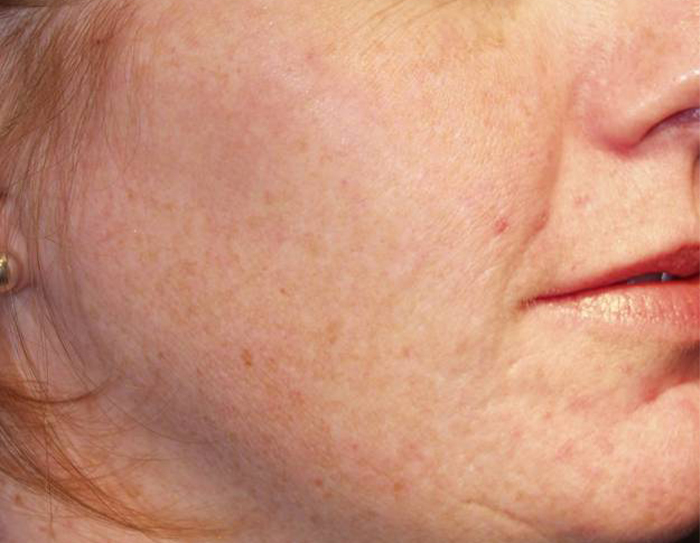
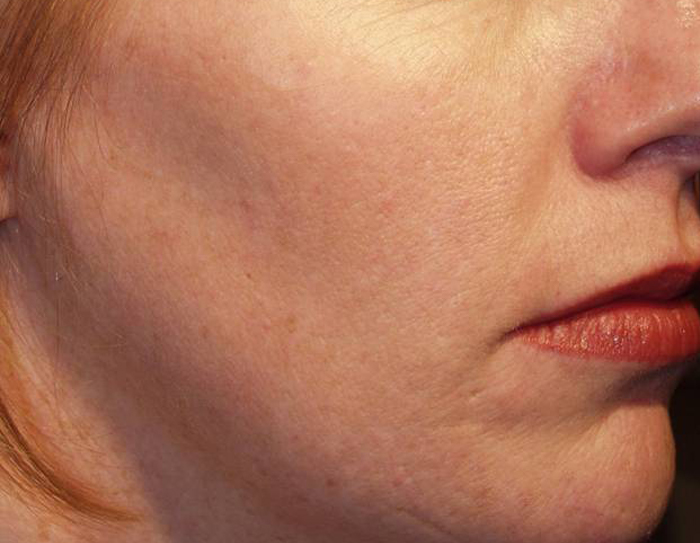
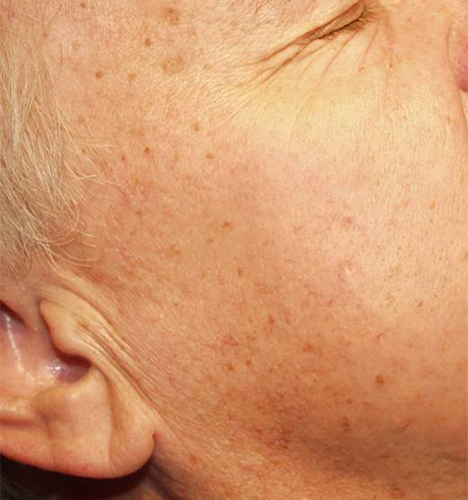
Melasma (muh-LAZ-muh) is a very common skin problem that causes brown to gray-brown patches on the face with sun exposure. It is most common in women and can affect the skin of the cheeks, nose, forehead, chin, and upper lip — typically in a distinctive pattern. It also can appear on other parts of the body that get lots of sun, such as the forearms and neck.
Quick Links
What Are the Causes of Melasma?
The cause of melasma remains unknown, but hormonal factors and exposure to sunlight are critical to its development. Melasma can occur without hormone pills or pregnancy—only 25% of women report melasma occurring after starting an oral contraceptive pill. Thus, melasma can occur with normal or endogenous hormone levels. Melasma should be considered a chronic disorder that, in many patients, lasts for years.
Melasma is a disorder of the pigment producing cells in our skin called melanocytes. Melanocytes are called dendritic cells and resemble what we might think of as an octopus shape with a central body and long tentacles or fingers stretching out from the central body. These tentacles or fingers of the melanocytes deposit pigment or melanin into the upper layer of our skin, the epidermis. The pigment is stored in small particles called melanosomes. Melasma-affected skin has increased melanocytes and melanocytes with more numerous dendrites or tentacles/fingers. Melanocytes of melasma-affected skin also show evidence of being more biologically active than melanocytes in normal or unaffected skin.
Some melasma has more pigment in the deeper skin layer or dermis, where the pigment is no longer in the melanocytes but in another cell called the melanophage, which is an inflammatory cell trying to remove pigment. This pigment in the deeper layer of the skin may explain why melasma is so difficult to eradicate.
It is still not known why certain areas of the face are predisposed to developing melasma while others are not involved. Hormone receptors, blood vessels, stem cell factors, and cutaneous nerves may play a role.

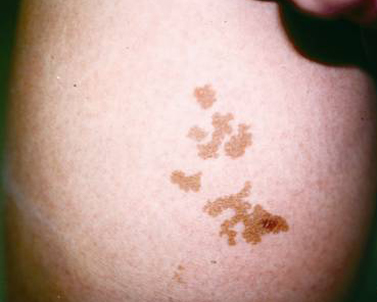
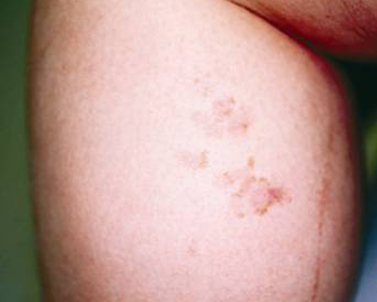
What Are Treatment Options for Melasma?
Treatment of melasma is very challenging, and even with excellent results from a treatment, the pigment of melasma can and very often does recur. If melasma develops after starting a hormone pill, it is recommended that the pill be stopped and all similar hormonal pills be avoided in the future; however, it is the experience of many melasma sufferers that the discoloration persists even after stopping all hormones.
I like to refer to this treatment pyramid which shows the steps of treatment — the first and most important is sun protection, then topical products and chemical peels and lastly laser treatments. The pyramid is an important symbol — even if laser treatment is selected, the base treatments of the pyramid — sun protection and topical products — must be maintained.
Sun Block and Sun Protection
The most basic and most essential part of any treatment regimen for melasma is daily -every single day, even cloudy days — use of a broad spectrum sun screen that contains a physical blocking agent — zinc or titanium dioxide. Unfortunately these sunscreens are not mass marketed to the public because the ingredients are more expensive and a little more difficult to formulate into a nice, pleasing product. Look for a sunblock that contains a zinc or titanium concentration of 5% or higher (this can be found on sunscreen label in active ingredients). Both of these products are microfine and meant to go on invisibly; however, titanium reflects visible light (not sun light) more than zinc so it looks more white on the skin surface. If you have darker skin and are worried about a white look then use a product with zinc rather than titanium as the active ingredient. Another active ingredient that is good for darker skin types is anthelios which is found in La Roche-Posay brand products.
Patients who wish to treat their melasma should employ additional methods of sun protection including avoiding sun as much as possible during the peak hours of the day, wearing a hat (and sun protective clothing if you have melasma on arms or chest), and seeking shade whenever possible.
Topical Products
Because melasma is a disorder of pigmentation, topical products that block the process of pigment production are helpful in the treatment of melasma. Pigment production is a complex process and there are many products that act at different steps in this process. No one product is 100% successful at preventing and treating pigment so often multiple different products are used as they all work at different steps in the process.
Retinoids
Retinoic acid and its derivatives (Retin-A, tretinoin, retinol, adapalene, tazaratene) have been shown to reduce the pigment of melasma and sun damage. They act by stimulating skin cell or keratinocyte turnover, decreasing transfer of pigment to skin cells and enhancing penetration of other active ingredients. Additionally, retinoids are an essential part of an anti-aging skin care regimen as they act to block the breakdown of collagen in the skin upon sun exposure.
Hydroquinone
Hydroquinone (HQ) is thought to improve pigment by inhibition of tryosinase, an enzyme critical for pigment production. It has been in use for over 50 years and has a long and well documented history of safety and efficacy in the treatment of pigment.
I often get questions about the safety of HQ because of things patients read online. I will summarize the controversy: Over the last several years, concern has been raised over the use of HQ. One concern is the development of ochronosis or blue-gray discoloration of the skin. In countries outside of the US, HQ was available without prescription in high concentrations and in combination with other products and ochronosis was more common with use of these products but is exceptionally rare with products approved for use in the US. Another of the concerns regarding HQ is the potential for risks from the production of benzene derivatives after hepatic metabolism; however, topically applied HQ is not metabolized by the liver and is water soluble and excreted thorough the kidneys. Kidney tumors are therefore a concern but no renal toxicity or tumors have ever been reported with topical HQ use.
HQ is a compound that is commonly found in many foods and beverages, including berries, tea, coffee, red wine, wheat, and the skin of pears. Workers involved in the manufacture of HQ and who are exposed to large quantities of this agent have not been found to have any significantly increased risk of premature death or increased prevalence of cancer and there has been no malignancy reported in animal testing. An extensive scientific review of HQ safety issues, found no risk real of malignancy and an exceedingly low risk of developing ochronosis or other side effects in patients using available prescription topical preparations of HQ under the supervision of a physician.
The best use of HQ is both to treat as well as prevent pigment darkening. For many patients, this means these products are best utilized in the high sun exposure months or prior to expected high sun exposure (tropical vacation or ski slopes). HQ should be used under the direction and supervision of a physician. A recommended practice is to take treatment breaks from HQ — meaning use for 3-6 months at a time and then stop use for 3-4 months. If there are any signs of skin irritation — such as redness, burning, itching -then HQ should be stopped for one or more applications before restarting use. It is important that skin is not irritated when trying to treat pigment.
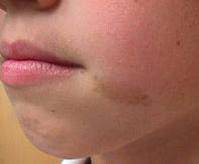
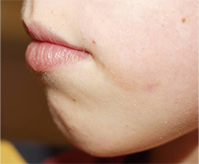
Combination Products
One of the most successful combination formulations has been 4% hydroquinone (HQ), 0.05% tretinoin, and 0.01% fluocinolone, in a cream called Tri-Luma®. Tri-Luma has recently become available again after being off the market for several years. It is recommended that if you use this cream, you take several-month breaks, as it contains a topical steroid, which can cause side effects on the skin with prolonged use.
Azeleic acid
Azelaic acid (AA) is a weak inhibitor of tyrosinase, the enzyme responsible for pigment production. It may also slow the growth of melanocytes and reduce free radical formation. AA is also effective for acne, so it is often used to treat acne, particularly in individuals with darker skin, due to its lightening properties.
Kojic acid
Kojic acid inhibits tyrosinase activity by binding to copper, a necessary cofactor for tyrosinase to function. It is probably the second most effective lightening agent after HQ but must be formulated in low concentration due to skin irritation.
Arbutin
Arbutin is derived from the bearberry plant and works as a lightening agent by inhibiting tyrosinase and another enzyme called DHICA, as well as blocking melanosome maturation. Arbutin has been studied more extensively for lightening sunspots than for treating melasma.
Ascorbic Acid or Vitamin C
In addition to being a powerful antioxidant, Vitamin C in skin serums and creams can block copper where it interacts with tyrosinase. Antioxidants are a critical part of any anti-aging program as they prevent oxidative injury to the skin with sun exposure.
Other topical agents
Licorice extract, soy, resveratrol, bearberry extract, emblica extract.


Schedule A Consultation
Integrating The Art of Medicine with the Science of Beauty
At Charlotte Skin & Laser, we offer personalized skincare with a boutique touch—combining medical expertise and aesthetic artistry to deliver natural, results-driven care. From skin checks to rejuvenation, our expert team is here to guide you.
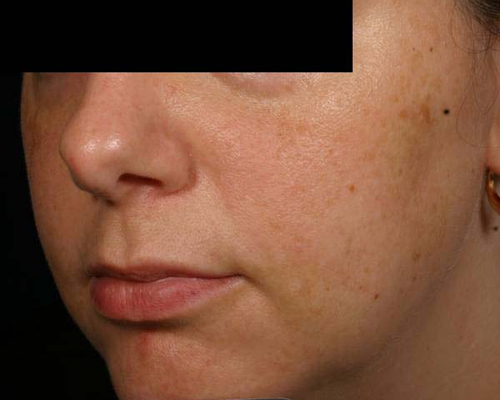
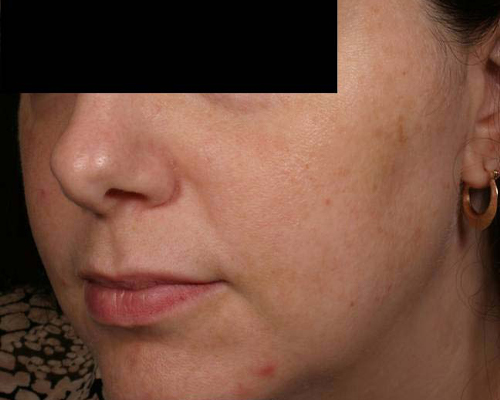
Chemical Peels
Chemical peels may improve or reduce the appearance of pigmentation caused by melasma, sun damage, acne, rashes, or other blemishes. However, because these peels can cause irritation, they must be used with caution and at lower strengths in patients with darker skin. Irritation or poor wound healing from a peel can lead to post-inflammatory hyperpigmentation (PIH), which is the darkening of the skin following inflammation.
Glycolic acid peels, particularly when combined with other ingredients, have shown the most benefit in treating melasma. Several proprietary peels, such as the Vi Peel, SkinCeuticals Pigment Balancing Peel, Perfect Peel, and CSL Renewal Peel, help lighten pigmentation.
For darker skin types, more treatments may be necessary because the pigment is more abundant and difficult to remove. Additionally, darker skin types are more prone to PIH caused by irritation from the peel, so lighter peel strengths must be used.
Lasers
A number of different lasers have been used in the treatment of melasma, but like topical agents and chemical peels, none are perfect. There is a very small risk of worsening melasma or increased darkening after laser treatments. Even in cases where the melasma fades beautifully after laser treatment, it remains prone to recurrence.
At Charlotte Skin & Laser, we have had the most success with the Fraxel Re:store or Fraxel Dual fractional non-ablative lasers with IPL (intense pulsed light).
It is critical to remember the pyramid nature of the treatment plan and not abandon the foundational treatments, such as sun protection and topical agents, even when starting chemical peels or laser treatments. Melasma should be viewed as a chronic condition, similar to high blood pressure, where control can be achieved but not a cure.
Relax and Refresh Your Skin With Melasma Treatment at Charlotte Skin & Laser
Melasma is a very challenging condition to treat and manage. At Charlotte Skin & Laser, we have helped many women improve their melasma and maintain healthier skin even if a permanent cure cannot be obtained. Charlotte Skin & Laser offers superior results and care designed to give you healthy, beautiful skin. Contact our office today at (704) 333-9113 or schedule your appointment online to get started with one of Charlotte’s premiere board-certified dermatologists, Dr. Elizabeth Rostan. Your most beautiful, healthiest skin starts here.